Our client, Mr C, an elderly man living with dementia, was admitted to hospital in August 2021 with cellulitis in the leg, which had failed to resolve at home taking oral Flucloxacillin. He was confirmed to have cellulitis at the hospital, immediately given IV antibiotics, and was deemed fit for discharge after a few days.
In many cases, pressure sores are wholly avoidable where good care is provided. Where care is provably substandard, you could make a pressure sore compensation claim.
Contents:
- How to make a claim for pressure sores?
- Can you sue a hospital for pressure sores?
- When can you make a claim for pressure sores?
- How long do I have to make a pressure sore claim?
- What are pressure sores?
- How much compensation for pressure sores?
- Will I have to go to court?
- Choosing the right solicitors for your pressure sore claim
- No Win, No Fee Pressure Sore Claims

According to the NHS, 1 in 20 people who are admitted to hospital with a sudden illness will go on to develop a pressure sore. This statistic alone means that it is important to be aware of what you can do if you have suffered as a result of developing a pressure sore.
How to make a claim for pressure sores?
To make a claim for pressure sores, it is best to speak with an experienced firm of medical negligence solicitors with experience in dealing with these types of claims.
You can contact our team to find out if you may have claim, and we can help you begin the process of outlining your claim and requesting any medical records that you may need.

Can you sue a hospital for pressure sores?
Strict NICE guidelines exist on the prevention and treatment of pressure ulcers, and where these are adhered to, it’s thought that 95% of cases are avoidable. Patients with mobility problems should always be frequently turned, and where ulcers do appear they should be monitored closely by staff, with at least one thorough check conducted each week. Medical staff should also ensure appropriate bedding is provided to ensure comfort for the patient and reduce the risks of bed sores occurring.
Where medical staff fail to observe these measures, and pressure sores develop or continue to deteriorate, leading to pain and suffering, you may be able to claim for pressure sores or bed sores to compensate you for the suffering and additional treatment that is required as a result.
When can you make a claim for pressure sores?
Serious pressure sores can be an indicator that there has been substandard care. This is because pressure sores can take time to develop, and should not happen if proper guidelines are being followed.
Where it can be proven that hospital or care home staff have caused, or worsened pressure sores, you can make a claim for pressure sore compensation.
How long do I have to make a pressure sore claim?
Generally speaking, you have 3 years from the moment you are aware of the negligent care towards you, that caused the pressure sore. After this time, it is extremely unlikely you will be able to make a claim.
There are exceptions to this limitation period, most notably if the person in question is under 18. If this is the case, then the 3-year limitation period will only begin once they turn 18. You can make a claim any time before this.
Limitation periods can be difficult to establish in cases, so if you’re unsure speak to one of our team today who can help you with your claim.
What are pressure sores?
Pressure sores are lesions or wounds that form around prominent bony areas of the body such as the hips, lower back, tailbone, heels, back of the head or elbows. They break down the skin around the area under ‘pressure’ and leave the underlying skin exposed.
Pressure sores can also be referred to as “bedsores” and “pressure ulcers.” The damage caused can range from discolouration of the skin to exposed muscle tissue or even bone.
Causes of pressure sores
Pressure sores develop when a person’s skin is in contact with a surface for an extended period of time. In a medical context, this can occur when a person is in a wheelchair or bed-bound for a sustained amount of time.
Where the skin is in contact with a hard surface, blood and therefore oxygen is restricted from reaching the skin tissue. If a person is not regularly moved to alleviate this pressure, the tissue at the affected site can begin to die.
Once an ulcer has begun to develop, an infection can occur, particularly if the area is moist or the person is more vulnerable to infection.
Grades of pressure sore
There are four grades of pressure sore.
Grade 1 – The wound is largely superficial, with the affected area of the skin appearing discoloured. If you have white skin the sore will appear red, whilst, in those with darker skin tones, it can appear blue or purple. Grade 1 sores will not turn white when pressure is applied and generally, the skin remains intact. The texture of the skin is unlikely to be affected, however, feeling warm, spongy or hard and general discomfort is commonplace as a result
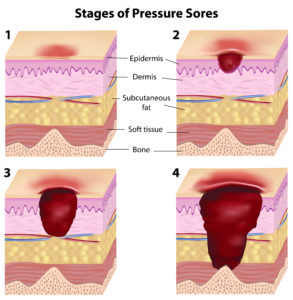
of itching or aching.
Grade 2 – Where the outer layer of skin (known as the “dermis”) is damaged, and skin has been lost. These pressure sores resemble an open wound or a blister.
Grade 3 – Multiple layers of skin are damaged and further damage has also been inflicted on the underlying tissues. Whilst muscle and bones remain unaffected, the injury comes to resemble a deep cut or cavity-like wound.
Grade 4 – The most severe form of pressure sore. Here the skin is so badly damaged that surrounding tissues begin to die (a condition known as “tissue necrosis”), and damage may also have occurred to underlying bone and muscle. These cases also carry the most significant risk of developing a serious and life-threatening infection.
Pressure Sore Negligence
In the more serious cases, those involving Grade 2, 3 or 4 pressure sores, there may be a strong argument for making a pressure sore claim due to the fact care may have been to a substandard level for a period of time long enough for the wounds to deteriorate to such an extent.
All bed sores can cause a great deal of pain and difficulty moving. Many take a long time to heal properly, and some may never heal at all. The elevated risk of infection can also lead to further health problems later, or delay recovery from their primary ailment.
Where clinical negligence on the part of hospital or care home staff can be proven to have caused or worsened any of the injuries related to pressure sores, regardless of the grade of the bed sore, you may be entitled to make a claim for compensation for you or your family member.
Related Articles
How much compensation for pressure sores?
As with all medical negligence claims, the amount of compensation you will receive for a pressure sore will vary depending on the severity of the injury, and your own personal circumstances.
Pressure sores can range in severity from a Grade 1, a mainly superficial wound, up to a Grade 4 which can expose bone and muscle tissue. The grade of the pressure sore will impact the amount of lasting damage that may be caused by the injury. A Grade 4 for example can lead to the need for limb amputation, which will severely impact a person’s ability to work in the future.
Furthermore, a person’s own circumstances will affect how much compensation they will receive. For example, if a person is no longer able to work, the amount of time until retirement age will be taken into consideration when giving compensation for a loss of earnings.
Blackwater Law client testimonial
Will I have to go to court?
In most pressure sore claims, you will not be required to go to court to receive compensation. In 2021 just over 3% of compensation claims needed to go to court to be resolved.
Most claims are settled out of court, so long as both parties can agree to a settlement amount. A claim will only need to go to court if there is a disagreement over the settlement amount or who is at fault for the claim.
You can learn more about when compensation claims go to court in this article.
I chose Blackwater Law straight away after just one phone call and I’ve never regretted it from that day to this.
Choosing the right solicitors for your pressure sore claim
It is essential to the success of your pressure sore claim that you choose the right medical negligence solicitor.
Having a solicitor that is experienced in dealing with the claim you are making, will lead to a smoother claim process, and may even be able to secure you more considerable compensation amount at the end.
Blackwater Law is ranked by The Legal 500 for both its experience in serious personal injury claims and medical negligence claims including pressure sores. Speak to one of our experienced solicitors today about your experience, and see if you have a claim.
Helpful Articles
No Win, No Fee Pressure Sore Claims
When you call us and receive free initial advice, if we believe you or your family member may be entitled to compensation, we will agree to represent you in your claim on a no-win, no-fee basis. This means that there is no risk to you. If your claim is unsuccessful, you will not have to pay any legal fees. Blackwater Law undertakes all medical negligence claims on a no-win, no-fee basis.





